Hospitals are Soviet-style Hellscapes Unfit for Humans
A Patient, Caregiver and Policy Manifesto
Everything that happened to my dying sister in that hospital was legal, standard, and indefensible.
She’d been in her local hospital for the past week. The giant tumor overtaking her pelvis had become unbearable with the weak pain management by her oncologist. So she went to the nearest ER and was admitted.
(Obviously a failure of medical oncology here, but that’s an article for another time).
She also happened to have a massive, radical surgery planned for the following week. They had already surgically bypassed her cancer-ridden colon in favor of a “stomach poop bag” as she called it. But this new surgery was going to go in to get the tumor out “for good.” Her bladder, uterus, vagina, cervix would all be removed in the process. Her confident surgeon said “we’re going for the ‘cure’ on this one,” so we were all hopeful.
(Obviously a failure of surgical oncology here, in imposing their wishful thinking on patients and loved ones, but that too is an article for another time.)
She would need to be strong to get through that.
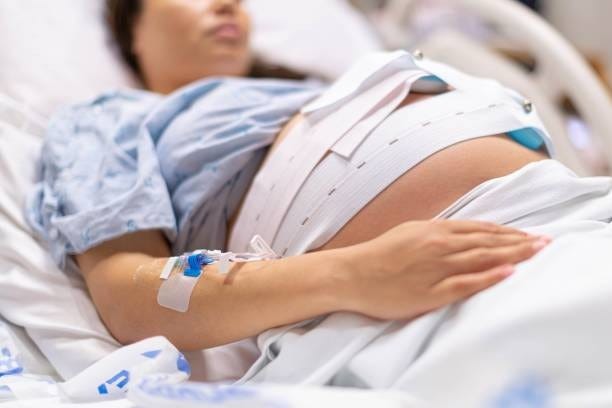
Since she couldn’t eat, couldn’t sleep and was fading quickly under the pain, she had made the rational choice to spend the week before her surgery in the hospital having her pain actively managed, and IV nutrition provided so that she could rest and prepare. It made some perverse sense in our degenerate system.
At the time, I was President Trump’s lead health advisor on the White House Domestic Policy Council. My career had been in health policy and public health. So I was a pretty informed and aggressive competent patient advocate.
The inpatient admission was largely a fail.
The meds were never adequate to manage her pain, there was never a doctor available to adjust them, the interventional pain specialist couldn’t come over to do the nerve block until most of the week was over - so she wasn’t resting. She was constantly interrupted by useless and unnecessary vitals checks (we can monitor the vitals of astronauts from space. What the hell with the interruptions?). Beeping. Announcements. Fluorescent lighting.
What she desperately did need - competent and timely pain management - was always too little, too late.
Her big surgery was taking place at the flagship facility of the system she was in, about a half-hour away. We assumed she’d be transferred the day before or the morning of, by ambulance. Two days before, we were informed she was going to be transferred that evening. I objected: by the time we arrived, the real doctors would be gone for the night, the transition wouldn’t be great, she’d had such a bad week already, and had only just gotten the nerve block that allowed her to rest.
Why not put off the transfer as long as possible? “Well, there’s a bed open now. We can’t guarantee that there will be a bed right before her surgery and if not, we’ll have to cancel her surgery (that she’d waited months for).”
I didn’t buy it.
They could transfer her straight to the surgery check-in the morning of and then she’d be admitted inpatient right after. They could transfer her early in the day tomorrow. There was no need to risk a bad transition for such a fragile patient who needed to rest. I called my sister’s surgeon, and her on-call colleague called me back. She assured me it would be fine - my sister’s pain meds wouldn’t wear off and would be managed - she’d make sure of it.
The ambulance was delayed and it was now the dead of night. I called her back pleading that she intervene - why couldn’t this wait until the morning when the hospital would be bustling with full clinical staff? She was mad at being awakened and implied I shouldn’t call her again.
What happened next was the worst night of my life.
My sister had many bad nights in her short life, so I can’t say if this was the worst for her, but if not, it was close.
The ambulance ride was unbearable. But that would likely have been true no matter when it happened. On arrival, there was no bed available in the surgical unit where she was supposed to be admitted, so they stashed her in some empty corner of the neurology floor.
To say the transition went badly would be an understatement.
There was no continuity of care. Nobody knew anything about her when she arrived. There was no doctor anywhere to be found. There were no pain meds. She might as well have been dumped at a bus stop.
She was screaming in agony, begging me to do something.
The nurses were apologetic but powerless to deliver an actual prescriber of any sort to the room. There was only one hospitalist in the entire building and he was busy in the ER. For hours.
I found this out because, like a crazy person, I literally ran from floor to floor of the entire hospital, trying to find an oncology or surgical wing where they knew how to manage pain. I went to every single nursing station demanding someone with prescribing power - crying, desperate, enraged, frantic. I was about 5 seconds from having security called on me.
None of it made a damned bit of difference.
I finally retreated back to my sister’s bedside, since, if she was going to suffer so much, the least I could do was be there and hold her hand. While I waited, I tweeted my rage, tagging the hospital. I called the chief lobbyist for the American Hospital Association - a wonderful human and longtime friend of our family - to try to get hold of the hospital’s leadership.
A few hours later, the doctor was freed up and prescribed the first pain meds my sister received in eight hours.
Early that morning, I stepped out to make some calls. When I came back, it was clear that that some of my overnight tweeting and networking had gotten through. The on-call surgeon I’d spoken to - she of the broken promises - and various hospital suits, were all crowded in my sister’s room. I was too broken and filled with white-hot fury to even speak.
If one of the most “powerful” health officials in the country couldn’t save a patient from this malpractice, what possible chance does anyone else have?
Hospitals don’t just torture us at the end of life - their mediocrities and incompetencies are on full display at the beginning of life too.
Last year, my daughter was due with her third baby.
She’d been induced with her first two babies, and so when her water broke naturally, she panicked. What does one do, when labor starts on its own, dear God in heaven?!
We showed up at the hospital about an hour later at 3 cm - the same dilation she’d been days before at her last prenatal visit. The right thing to do? Send her home to labor naturally until things got real. That’s what they used to do, decades ago. But then babies might accidentally, you know, come out without the hospital cash register dinging in the background.
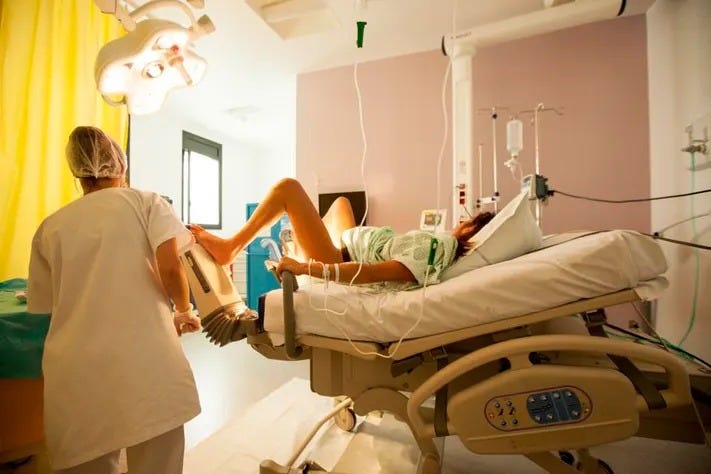
So, instead, they strap her in. First the IVs. Why can’t she feed and hydrate herself? She’s completely healthy. Oh right, because the c-section rate is so disgracefully high in this country that they starve laboring women for hours and hours on the not-so-off chance that they end up in surgery.
Then the fetal monitor which, despite our ability to land on the moon, is completely beyond our powers to keep in place on a big belly. Constant interruptions because the stupid monitor strap has moved.
Why do you need to monitor? This is a low-risk, no-drama situation.
“It’s protocol.”
What is the evidence of fetal monitoring improving outcomes rather than hastening the imposition of dangerous interventions?
Blank stare. “It’s protocol.”
What if she refuses?
“She can’t. It’s protocol.”
No really, what if she refuses?
“She can’t deliver here.”
So she can just walk out of here?
“Well, we’d have to call CPS.”
Ah yes, the CPS card.
And so, like clockwork, the cascade of interventions began. First, of course, since she wasn’t actually in active labor (remember the 3 cm?), she was just sitting there for a few hours while nothing happened. Taking up a bed. Unacceptable.
The right thing to do? Send her home to labor naturally until things got real. That’s what they used to do, decades ago. But then babies might accidentally, you know, come out without the hospital cash register dinging in the background.
Time for “augmentation.” That’s when they jack you up with pitocin - a synthetic counterfeit of the natural hormone oxytocin that is responsible for regulating uterine contractions to correspond with the rest of the hormonal symphony present in physiological birth (which no L&D doctor or nurse has ever actually observed).
Pitocin, unlike oxytocin, doesn’t wax and wane with the needs of the bodies involved, and instead just asserts itself aggressively and immediately. Unnatural, shocking, and unbearable contractions start within 30-60 minutes. Not the natural kind that gradually grow and build on each other, productively moving the baby when the rest of the body is ready.
My daughter was no exception. And so of course, the epidural.
The vast majority (like 80-90 percent) of women given pitocin end up with an epidural - almost 25-50 percent more than those not given pitocin.
Epidurals stop or slow the contractions. And often the baby’s heart rate. Failure to progress. Fetal distress. So then, emergency c-section. See how this works?
I’m sure it has nothing to do with how the hospital makes more money if they can move women through the process in 12 hours, ending with a (dangerous, expensive) invasive surgery, and on to the next lady. Rather than sitting with a mother’s labor for the 48-72 hours it might naturally take under the oxytocin-suppressing hospital conditions.
Every mammal on earth retreats to dark, enclosed, solitude to birth their young.
That is the optimal environment of safety that signals their hormonal symphony to get to work. Any bright light, interruption or the slightest stress (caused by observation of others, noises in the woods, etc) causes cortisol to spike. Cortisol shuts off oxytocin. Uterine contractions slow or stop until the animal is safe again.
“Well, we’d have to call CPS.” Ah yes, the CPS card.
So you can imagine the cortisol/oxytocin impact of bright, fluorescent lighting, beeping, constant interruptions, monitoring, observation, and an entire culture built around fear-mongering this process as a medical, life-threatening emergency.
No wonder we have the highest, most disgraceful, most scandalous c-section rate of any nation on earth. Babies don’t come out easily under these conditions.
In my daughter’s case, that wasn’t going to happen. That’s why I was there.
Even still, after my granddaughter was born without a c-section, the shenanigans continued.
Mom and baby were moved up to a different unit at 1:00 am, naturally exhausted and wanting to just snuggle and sleep. The new nurse comes in with a clipboard and insists on explaining how we need to keep track on this complex chart of the timing and amount of each poop and pee drop, each feeding, for how long, on which boob, and we have to make sure there’s no feeding the baby within an hour of the three-hour glucose heel-prick, and on and on.
The nurse was actually surprised and butt-hurt when we told her, politely, to buzz off.
We will not be doing your chart-tracking. We will not be following your instructions. Leave us alone until morning.
They did not comply. That night was so miserable for my daughter, with the beeping and lighting and constant interruptions, she got no rest. In the morning, she had decided that it was neither good for her nor her daughter to spend another night there. Even though the hospital revenue model “protocol” demanded two nights.
Thank goodness I had warned her about the CPS card before they played it, or she might have buckled in shock. But she was prepared, and I was never so proud as when she stood her ground. We left that afternoon.
They did call CPS. Because, of course they did.
My daughter swatted that away later, but the totalitarianism of the mindless, and often dangerous hospital rituals knows no bounds.

Every family has these stories, to our nation’s great and calamitous shame.
My father’s heart condition means my family has spent many, many hours, days and weeks observing the bureaucratic banalities of a Soviet-style system:
Patient menus and cafeterias with nothing but processed, pesticide-soaked offerings. Heart patients are forbidden to order steak but required to consume “heart-healthy” concoctions riddled with seed oils, sugar, petroleum-based food dyes and refined carbs.
Windows locked to exclude fresh air, unfiltered sunlight and the healing sounds of birds and rustling leaves.
Dehumanizing prison garb for patients that strips them of their dignity, warmth and comfort.
Protocols written by lawyers rather than humans, such as “fall prevention” implemented as heart-attack-inducing alarm-blaring and stern ninnying from nurses, when a grown-up dares to rise from a bed.
Disrupted rest in the form of hourly vitals checks, beeping machines that alarm if a tube twists wrong, fluorescent lighting that can’t be fully turned off.
The pretense of clinical oversight without the presence of actual clinical oversight. Armies of scrub-wearers constantly circling, but disempowered to adjust prescriptions and dietary orders, waive senseless protocols, and otherwise exercise discretion. This is particularly egregious in the off-hours, when it’s not uncommon for a facility to have one clinical decision-maker onsite.
Revenue-driven and convenience-driven protocols such as drugging or cutting a baby out of its mother prematurely, or transferring medically fragile patients overnight unnecessarily.
Death-by-hospital:
Between 44,000-98,000 preventable deaths per year.
A maternal mortality rate more than twice the average of developed nations - four or five times the rate of many of our peer nations, as well as 25 percent higher infant mortality than the average for developed countries. (OECD)
Almost 2 million hospital-acquired infections per year, killing 100,000 patients. (CDC)
In short, this is a business model that should be burned to the ground. It is unfit for human participation. It is incompatible with health or healing.
Hospitals do not provide health care. They’re where you go when health care has already failed.
They monetize and capitalize on our extinction-level chronic illness rates. They invent reasons for their own existence, such as convincing the world that mammalian birth is a medical emergency. They have to threaten you with the government stealing your children just to keep you there.
In short, this is a business model that should be burned to the ground. It is unfit for human participation. It is incompatible with health or healing.
There is an important caveat here: mechanics.
When you have a bullet in your belly, a third-degree burn, or a bone sticking out, you need a skilled mechanic waiting in the OR next to the ER. When you’re having a stroke or a heart attack, an American ER is just the place to be. When one of those patients doesn’t make it, you want their organs transplanted into someone who might, waiting in the OR down the hall.
There might be a few other use cases I’ve forgotten, but by and large, that’s it. The rest of the giant compound sitting on multiple acres of tax-free real estate is just a profit center of misery, selling a false sense of blue-lit security.
The life-saving, acute services that are valuable are not profitable. They cannot be made profitable.
They require an expensive crew of high-skill labor, cutting edge technology, the most expensive forms of ground and air transport, with 24/7/365 access for a catchment area that does not produce enough of these needs each year to recoup costs.
The rest of the hospital complex has been created to subsidize it.
Growing year over year, the amount of high-cost stuff done to sick people is where the profit is. Stuff that doesn’t have to be done in a hospital. Stuff that turns out worse when the abusive culture of a hospital is infused into patient experience.
When ten people with broken bodies arrive at an ER after a multi-car pileup, the protocols and procedures must be rigid and enforced, because there’s no time and no room for error. This is the theory behind military discipline, whether in Fallujah or your local trauma bay - where the stakes are so high and the crisis so kinetic.
But that culture of top-down authoritarianism loses all appropriateness and perspective when the stakes are routine, such as elective surgeries, cancer palliation, birthing babies. Nonetheless, the culture created for the trauma context infuses the entire complex so overwhelmingly as to inhibit or reverse healing and health rather than protect it.
Not to mention the cost.
What cannot be sustained will not be.
Fortunately, technology is emerging just in time to save us from these totalitarian bureaucracies we call “health” systems.
Increasingly, the hospital is being unbundled into solutions that are based at home, where value is rewarded in the form of greater dignity, comfort, nourishing food, incandescent lighting, and peace and quiet (or the health-promoting chaos of grandkids and goldendoodles). This model promises to produce better outcomes than the overpriced, Soviet-style hellscape we’ve been tolerating.
Decentralized solutions and vendors are now able to bill your health plan for true hospital-level care in the home: IV antibiotics, oxygen, imaging, daily physician oversight. Tools like continuous glucose monitors, Holter monitors and cardiac patches, and wearables like Oura rings turn episodic vital-sign snapshots into continuous streams of data. We’re even starting to be able to do imaging with handheld devices at home. Home-based lab draws are already becoming mainstream.
Tele-ICUs, at-home monitoring, virtual-first care models, predictive algorithms that detect deterioration before crisis - all of it is overthrowing the hospital-based religious cult that has us cowed in our paper gowns with our butts hanging out.
Right-sizing hospitals to true emergencies and intensive rescue will destroy their business model. It will preserve the least profitable services and replace the most profitable ones with more efficient, more humanity-compatible models in the home and community where healing is far more likely and affordable.
Policy-makers will need to decide what that means.
Maybe if we’re not subsidizing the behemoth, tax-exempt compounds charging facility fees for routine care, we’ll be able to more generously subsidize the urban and rural ERs that are struggling to keep their doors open.
This transformation can’t happen fast enough.
Between the predatory collections and billing practices I wrote about in my last piece, and the soulless torment of fragile patients like my sister, the world would be better without the vast majority of what hospitals are inflicting on us every day.
But dismantling a failing system requires more than my white-hot fury.
It requires reimbursement reform that stops cross-subsidizing bureaucratic sprawl.
It requires site-neutral payments that end the incentive to drag routine care into the most expensive square footage in America.
It requires regulatory relief that allows hospital-at-home models, independent surgical centers, community birth centers, home birth attendants, and virtual-first care to compete on equal footing.
And it requires political courage. Hospitals are usually the largest employer in every congressional district. Protecting their current business model is not the same thing as protecting patients.
We do not have to accept the ungodly status quo as the price of modernity. We do not have to confuse bureaucracy with safety, or institutional control with care. Systems built by human beings can be dismantled and rebuilt by human beings - this time around dignity, autonomy, and actual healing.
All Soviet empires must fall.








I have hope that we are at a turning point. At least I pray that we are. Thanks for sharing your stories Katy.
I read this with my stomach clenched, as the most haunting parts aren’t “rare horror stories”, but they’re the fact that so much of what you describe is ordinary, billable, policy-compliant reality: the overnight transfer because “a bed is open”, the vanishing prescriber at 2 a.m., the relentless vital checks that ignore sleep as treatment, and a culture where “protocol” substitutes for judgment. 
Your sister’s night exposes the most dangerous illusion in modern inpatient care: that a building full of staff equals continuous clinical oversight. When pain control, delirium prevention, and basic human needs depend on a single overstretched decision-maker (or none at all), the system can look busy while the patient is effectively abandoned. That gap, between “we have policies” and “someone with authority is actually accountable in real time”, is where suffering multiplies. 
And the childbirth story hits another nerve: the way hospital environments can be inherently anti-physiologic. Bright light, noise, constant surveillance, immobilization, coercive threats (“CPS”), and cascade-style interventions don’t just create emotional distress, but they can change labor dynamics through stress physiology in ways that end up being blamed on the mother’s body. Even if readers disagree with some of the rhetoric, the lived experience you’re pointing to is real: too many “routine” processes are designed around throughput, liability, and documentation rather than rest, autonomy, and outcomes that matter to families. 
What I hope people take from this is not just rage (though the rage is earned), but a clear agenda. If hospitals want to call themselves healing institutions, a few non-negotiables rise to the top:
1. Continuous clinical responsibility for high-risk symptoms like severe pain, meaning timely prescribing authority, not just sympathetic bedside apologies.
2. Sleep, light, and noise as core vital signs (and interruptions justified by evidence, not habit).
3. Protocols with an “off-ramp”, a way for clinicians to document a reasoned exception and for patients to refuse non-essential interventions without punishment.
4. Transparent accounting of harms (iatrogenic events, infections, preventable deaths) tied to real consequences and incentives to improve, not PR. 
Thank you for writing this so plainly.